Analisi delle esperienze e comportamenti dei fisioterapisti rispetto alla tematica dei confini professionali: uno studio pilota
Analysis of the experiences and behaviors of physiotherapists with regards to the issue of professional boundaries: a pilot study
Autori
Gianmarco Gioia (Physiotherapist, MSc – Az. USL Toscana Centro)
Simone de Luca (Physiotherapist, MSc – Department of Neurosciance, Rehabilitation, Ophthamology, Genetics and Mathernal Infantile Sciences (DINOGMI), University of Genova Campus of Savona, SV, Italy)
Elia Bassini (Physiotherapist, MSc – 1) Az USL Umbria 2; 2) University of Rome Tor Vergata)
Cristiana Conti (Sport Psichologist, Psychotherapist, PhD – Private Practice, Florence)
Sara Biondi (Sport Psychologist – Private Practice, Rome)
Patrizia Galantini (Physiotherapist, Msc – University of Florence)
Giacomo Rossettini (Physiotherapist, PhD – Department of Physiotherapy, Faculty of Sport Sciences, Universidad Europea de Madrid, Villaviciosa de Odòn, Spain)
Antonello Viceconti (Physiotherapist, PhD – Private Practice, Savona)
Introduction
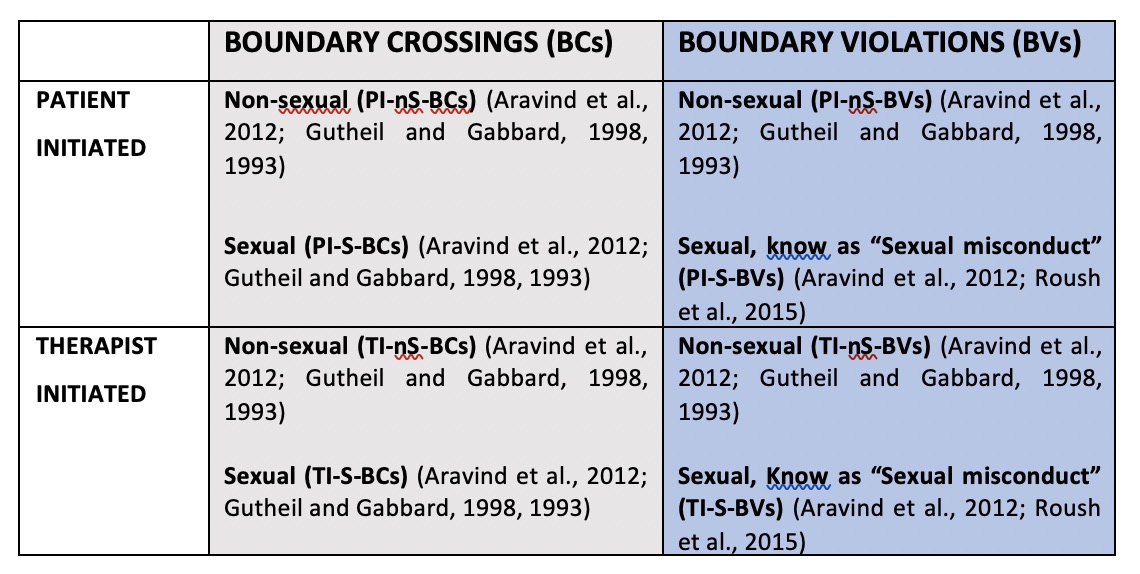
Given the nature of their professional role, physiotherapists tend to establish an intimate relationship with patients. This condition may rise ethical and professional issues: patients and physical therapists, may less likely aware of the importance of professional boundaries within the therapeutic relationship. As a result, they may lose the ability to recognize the “crossings” of professional boundaries, and counteract the consequences or conversely, they may be themselves the initiators of behaviours that may represent a violation of professional boundaries.
Methods
A research project has been structured to explore experiences, attitudes, and behaviours in the field of sexual crossings and violations of professional boundaries in the population of Italian physiotherapists and students. The entire project has been structured into two lines of research concerning:1) physiotherapy students;2) licensed physiotherapists. For this degree Thesis, the first phase of the research line concerning students is described. This step involves the writing of a research protocol regarding a cross-sectional observational study in which has been investigated the prevalence of patient-initiated sexual crossings and violations and the strategies that students used to manage any infractions that may have occurred. It has also been reported the results of the pilot study that was conducted on a convenience sample of 16 students with the purpose of 1) testing the feasibility of the designed cross-sectional study and 2) obtaining feedback from participants regarding the questionnaire developed. The survey was administered using the Survey Monkey online tool.
Results
A sample of 16 participants was recruited from students in the second and third year of the Bachelor in Physiotherapy at the University of Florence (Italy). Given the low sample size, only a descriptive statistical analysis was performed. The Response Rate of the questionnaire on sexual violations of professional boundaries was n = 12 out of 16, 75%. All participants who completed the evaluation and feedback questionnaire (n = 10 out of 16, 62,5%) took less than 15 minutes to complete the boundary violation questionnaire and all of them (n = 10 out of 10, 100%) reported agreement on the clarity, comprehensibility and appropriateness of the proposed questions concerning the study’s purpose of inquiry. Seven out of twelve subjects who completed the questionnaire on sexual violations of professional boundaries (n = 7 out of 12, 58.33%) reported having experienced at least once in their academic careers a sexual violation of professional boundaries initiated by their patients. Only 25% of the participants (n = 3 out of 12, 25%) reported that they had received training on the topic of professional boundaries of a sexual nature. The entire sample of students (n = 12 out of 12, 100%) would find useful for their professional careers to conduct specific training in this regard.
Discussion and Conclusion
The pilot study conducted represented the first step in the entire planned research project and confirmed the feasibility and relevance of the instrument to be used concerning the phenomenon under study. In line with the existing literature, these preliminary data show a considerable prevalence of sexual violations of professional boundaries initiated by patients to physiotherapy students. These results point to deepening the issue of professional boundary violation on a larger sample of students through the cross-sectional observational study whose protocol was presented.
REFERENCES
AIFI, 2011. Codice Deontologico | A.I.FI. [WWW Document]. https://aifi.net/. URL https://aifi.net/professione/codice-deontologico/ (accessed 1.21.24).
Amanulla, S., Saju, I., Solé, S., Campoy, C., Martínez, L., Pérez-Yus, M.C., Sitjà-Rabert, M., Serrat, M., Bravo, C., Lo, K., 2021. Inappropriate Patient Sexual Behavior in Physiotherapy: A Systematic Review. Sustainability 13, 13876. https://doi.org/10.3390/su132413876
Ang, A.Y.-C., DipPhys, I.C.G., DipPhys, S.J.G., 2010. Sexual professional boundaries: physiotherapy students’ experiences and opinions 38.
APTA, 2019. Standards of Ethical Conduct for the Physical Therapist Assistant [WWW Document]. URL https://www.apta.org/apta-and-you/leadership-and-governance/policies/standards-of-ethical-conduct-for-the-physical-therapist-assistant (accessed 1.15.24).
Aravind, V.K., Krishnaram, V.D., Thasneem, Z., 2012. Boundary Crossings and Violations in Clinical Settings. Indian J Psychol Med 34, 21–24. https://doi.org/10.4103/0253-7176.96151
Boissonnault, J.S., Cambier, Z., Hetzel, S.J., 2019. Inappropriate Patient Sexual Behavior When Working in Sensitive Areas of the Body: Results From a National Physical Therapy Survey. The Journal of Women’s & Pelvic Health Physical Therapy 43, 36. https://doi.org/10.1097/JWH.0000000000000118
Boissonnault, J.S., Cambier, Z., Hetzel, S.J., Plack, M.M., 2017. Prevalence and Risk of Inappropriate Sexual Behavior of Patients Toward Physical Therapist Clinicians and Students in the United States. Physical Therapy 97, 1084–1093. https://doi.org/10.1093/ptj/pzx086
Bowen, E., Nayfe, R., Milburn, N., Mayo, H., Reid, M.C., Fraenkel, L., Weiner, D., Halm, E.A., Makris, U.E., 2020. Do Decision Aids Benefit Patients with Chronic Musculoskeletal Pain? A Systematic Review. Pain Med 21, 951–969. https://doi.org/10.1093/pm/pnz280
Bütow-Dûtoit, L., Eksteen, C.A., De Waal, M., Owen, J.H., 2006. Sexual harassment of the physiotherapist in South Africa. South African Journal of Physiotherapy 62, 9–12. https://doi.org/10.4102/sajp.v62i4.160
Cambier, Z., 2013. Preparing New Clinicians to Identify, Understand, and Address Inappropriate Patient Sexual Behavior in the Clinical Environment: Journal of Physical Therapy Education 27, 7–14. https://doi.org/10.1097/00001416-201301000-00003
Cambier, Z., Boissonnault, J.S., Hetzel, S.J., Plack, M.M., 2018. Physical Therapist, Physical Therapist Assistant, and Student Response to Inappropriate Patient Sexual Behavior: Results of a National Survey. Physical Therapy 98, 804–814. https://doi.org/10.1093/ptj/pzy067
Caneiro, J.P., Bunzli, S., O’Sullivan, P., 2021. Beliefs about the body and pain: the critical role in musculoskeletal pain management. Braz J Phys Ther 25, 17–29. https://doi.org/10.1016/j.bjpt.2020.06.003
Celenza, 2007. Sexual Boundary Violations: Therapeutic, Academic, and Supervisory Contexts [WWW Document]. URL https://www.andreacelenza.com/sexual-boundary-violations-therapeutic-academic-and-supervisory-contexts/ (accessed 2.19.24).
College of Psychologist of Ontario, 2024. Professional Boundaries in Health-Care Relationships – CPO Public. URL https://cpo.on.ca/cpo_resources/professional-boundaries-in-health-care-relationships/ (accessed 1.20.24).
Cooper, I., Jenkins, S., 2008. Sexual boundaries between physiotherapists and patients are not perceived clearly: an observational study. Australian Journal of Physiotherapy 54, 275–279. https://doi.org/10.1016/S0004-9514(08)70007-2
Cooper, I., Jones, A., Jenkins, S., 2010. Professional sexual boundaries—Asian and Western perception: An observational study. Hong Kong Physiotherapy Journal 28, 2–10. https://doi.org/10.1016/j.hkpj.2010.11.003
Cullen, R.M., 1996. Sexual contact in the professional relationship : the 1996 survey of NZSP members [WWW Document]. New Zealand journal of physiotherapy,NZ journal of physiotherapy Aug 1997; v.25 n.2:p.7-9; issn: URL https://natlib.govt.nz/records/21056446 (accessed 1.15.24).
Cummings, N., 1992. Self-defense training for college women. J Am Coll Health 40, 183–188. https://doi.org/10.1080/07448481.1992.9936280
de leeuw, E., Hox, J., Dillman, D., 2008. International Handbook Of Survey Methodology (2008).
deMayo, R.A., 1997. Patient Sexual Behaviors and Sexual Harassment: A National Survey of Physical Therapists. Physical Therapy 77, 739–744. https://doi.org/10.1093/ptj/77.7.739
Eysenbach, G., 2004a. Tackling Publication Bias and Selective Reporting in Health Informatics Research: Register your eHealth Trials in the International eHealth Studies Registry. J Med Internet Res 6, e35. https://doi.org/10.2196/jmir.6.3.e35
Eysenbach, G., 2004b. Improving the Quality of Web Surveys: The Checklist for Reporting Results of Internet E-Surveys (CHERRIES). Journal of Medical Internet Research 6, e132. https://doi.org/10.2196/jmir.6.3.e34
Fitzgerald, L.F., Shullman, S.L., Bailey, N., Richards, M., Swecker, J., Gold, Y., Ormerod, M., Weitzman, L., 1988. The incidence and dimensions of sexual harassment in academia and the workplace. Journal of Vocational Behavior 32, 152–175. https://doi.org/10.1016/0001-8791(88)90012-7
Garfinkel, P.E., Dorian, B., Sadavoy, J., Bagby, R.M., 1997. Boundary violations and departments of psychiatry. Can J Psychiatry 42, 764–770. https://doi.org/10.1177/070674379704200710
Geri, T., Viceconti, A., Minacci, M., Testa, M., Rossettini, G., 2019. Manual therapy: Exploiting the role of human touch. Musculoskelet Sci Pract 44, 102044. https://doi.org/10.1016/j.msksp.2019.07.008
Glass, L.L., 2003. The gray areas of boundary crossings and violations. Am J Psychother 57, 429–444. https://doi.org/10.1176/appi.psychotherapy.2003.57.4.429
Grieco, A., 1987. Scope and nature of sexual harassment in nursing. Journal of Sex Research 23, 261–266. https://doi.org/10.1080/00224498709551362
Gutheil, T.G., Gabbard, G.O., 1998. Misuses and misunderstandings of boundary theory in clinical and regulatory settings. Am J Psychiatry 155, 409–414. https://doi.org/10.1176/ajp.155.3.409
Gutheil, T.G., Gabbard, G.O., 1993. The concept of boundaries in clinical practice: theoretical and risk-management dimensions. Am J Psychiatry 150, 188–196. https://doi.org/10.1176/ajp.150.2.188
Harvie, D.S., Meulders, A., Madden, V.J., Hillier, S.L., Peto, D.K., Brinkworth, R., Moseley, G.L., 2016. When touch predicts pain: predictive tactile cues modulate perceived intensity of painful stimulation independent of expectancy. Scand J Pain 11, 11–18. https://doi.org/10.1016/j.sjpain.2015.09.007
Higgs, J., Refshauge, K., Ellis, E., 2001. Portrait of the physiotherapy profession. J Interprof Care 15, 79–89. https://doi.org/10.1080/13561820020022891
Hiller, A., Guillemin, M., Delany, C., 2015. Exploring healthcare communication models in private physiotherapy practice. Patient Educ Couns 98, 1222–1228. https://doi.org/10.1016/j.pec.2015.07.029
Hoffmann, T., Bakhit, M., Michaleff, Z., 2022. Shared decision making and physical therapy: What, when, how, and why? Braz J Phys Ther 26, 100382. https://doi.org/10.1016/j.bjpt.2021.100382
Hotelling, K., 1991. Sexual harassment: A problem shielded by silence. Journal of Counseling & Development 69, 497–501. https://doi.org/10.1002/j.1556-6676.1991.tb02631.x
Johnson, C., Knight, C., Alderman, N., 2006. Challenges associated with the definition and assessment of inappropriate sexual behaviour amongst individuals with an acquired neurological impairment. Brain Inj 20, 687–693. https://doi.org/10.1080/02699050600744137
Jorgenson, L.M., Hirsch, A.B., Wahl, K.M., 1997. Fiduciary duty and boundaries: Acting in the client’s best interest. Behavioral Sciences & the Law 15, 49–62. https://doi.org/10.1002/(SICI)1099-0798(199724)15:1<49::AID-BSL253>3.0.CO;2-X
Knapp, S., Slattery, J.M., 2004. Professional Boundaries in Nontraditional Settings. Professional Psychology: Research and Practice 35, 553–558. https://doi.org/10.1037/0735-7028.35.5.553
Lehmann, 2019. Combatting Sexual Harassment and Inappropriate Patient Sexual Behavior [WWW Document]. APTA. URL https://www.apta.org/apta-magazine/2019/02/01/combatting-sexual-harassment-and-inappropriate-patient-sexual-behavior (accessed 2.19.24).
Lin, I., Wiles, L., Waller, R., Caneiro, J.P., Nagree, Y., Straker, L., Maher, C.G., O’Sullivan, P.P.B., 2020. Patient-centred care: the cornerstone for high-value musculoskeletal pain management. Br J Sports Med 54, 1240–1242. https://doi.org/10.1136/bjsports-2019-101918
McComas, J., Hébert, C., Giacomin, C., Kaplan, D., Dulberg, C., 1993. Experiences of Student and Practicing Physical Therapists With Inappropriate Patient Sexual Behavior. Physical Therapy 73, 762–769. https://doi.org/10.1093/ptj/73.11.762
McComas, J., Kaplan, D., Giacomin, C., 1995. Inappropriate patient sexual behaviour in physiotherapy practice: a qualitative analysis of questionnaire comments. Physiother Can 47, 127–133.
McParlin, Z., Cerritelli, F., Rossettini, G., Friston, K.J., Esteves, J.E., 2022. Therapeutic Alliance as Active Inference: The Role of Therapeutic Touch and Biobehavioural Synchrony in Musculoskeletal Care. Front Behav Neurosci 16, 897247. https://doi.org/10.3389/fnbeh.2022.897247
Miciak, M., Mayan, M., Brown, C., Joyce, A.S., Gross, D.P., 2019. A framework for establishing connections in physiotherapy practice. Physiotherapy Theory and Practice 35, 40–56. https://doi.org/10.1080/09593985.2018.1434707
NCSBN, 1998. A Nurse’s Guide to Professional Boundaries [WWW Document]. NCSBN. URL https://www.ncsbn.org/brochures-and-posters/a-nurses-guide-to-professional-boundaries (accessed 1.15.24).
O’Sullivan, V., Weerakoon, P., 1999. Inappropriate sexual behaviours of patients towards practising physiotherapists: a study using qualitative methods. Physiotherapy Res Intl 4, 28–42. https://doi.org/10.1002/pri.1999.4.1.28
Physiotherapy Board of New Zealand, 2023. Professional boundaries standard [WWW Document]. Mercury IT. URL https://www.physioboard.org.nz/standards/physiotherapy-standards/professional-boundaries-standard (accessed 1.20.24).
Plaut, S., 2008. Sexual and nonsexual boundaries in professional relationships: Principles and teaching guidelines. Sexual and Relationship Therapy 23, 85–94. https://doi.org/10.1080/14681990701616624
Pope, K.S., Vasquez, M.J., 2007. Ethics in Psychotherapy and Counseling: A Practical Guide. John Wiley & Sons.
Poulis, I., 2007. Bioethics and physiotherapy. J Med Ethics 33, 435–436. https://doi.org/10.1136/jme.2007.021139
RHPA, 1991. Regulated Health Professions Act [WWW Document]. Ontario.ca. URL https://www.ontario.ca/laws/view (accessed 3.15.24).
Roger, J., Darfour, D., Dham, A., Hickman, O., Shaubach, L., Shepard, K., 2002. Physiotherapists’ use of touch in inpatient settings. Physiother Res Int 7, 170–186. https://doi.org/10.1002/pri.253
Rondoni, A., Rossettini, G., Ristori, D., Gallo, F., Strobe, M., Giaretta, F., Battistin, A., Testa, M., 2017. Intrarater and Inter-rater Reliability of Active Cervical Range of Motion in Patients With Nonspecific Neck Pain Measured With Technological and Common Use Devices: A Systematic Review With Meta-regression. J Manipulative Physiol Ther 40, 597–608. https://doi.org/10.1016/j.jmpt.2017.07.002
Roush, S.E., Cox, K., Garlick, J., Kane, M., Marchand, L., 2015. Physical therapists’ perceptions of sexual boundaries in clinical practice in the United States. Physiotherapy Theory and Practice 31, 327–336. https://doi.org/10.3109/09593985.2014.1003420
Sanbar et al., A., 2007. The Medical Malpractice Survival Handbook.
Soundy, A., Stubbs, B., Jenkins, S., Cooper, I., 2013. Sexual professional boundaries perceived by undergraduate and graduate physiotherapists: A cross sectional survey. Physiotherapy 99, 298–304. https://doi.org/10.1016/j.physio.2012.12.005
SurveyMonkey, 2024. SurveyMonkey: lo strumento di indagine on-line gratuito più popolare al mondo [WWW Document]. SurveyMonkey. URL https://it.surveymonkey.com/ (accessed 2.24.24).
Tangri, S.S., Burt, M.R., Johnson, L.B., 1982. Sexual harassment at work: Three explanatory models. Journal of Social Issues 38, 33–54. https://doi.org/10.1111/j.1540-4560.1982.tb01909.x
TSRM PSTRP, 2021. Costituzione-etica-FNO-TSRM-e-PSTRP-def.pdf [WWW Document]. URL https://www.tsrm-pstrp.org/wp-content/uploads/2021/11/Costituzione-etica-FNO-TSRM-e-PSTRP-def.pdf (accessed 1.21.24).
University of Manitoba, 1988. Sexual Harassment Questionnaire.
von Elm, E., Altman, D.G., Egger, M., Pocock, S.J., Gøtzsche, P.C., Vandenbroucke, J.P., STROBE Initiative, 2014. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) Statement: guidelines for reporting observational studies. Int J Surg 12, 1495–1499. https://doi.org/10.1016/j.ijsu.2014.07.013
Walker, S.C., Trotter, P.D., Swaney, W.T., Marshall, A., Mcglone, F.P., 2017. C-tactile afferents: Cutaneous mediators of oxytocin release during affiliative tactile interactions? Neuropeptides 64, 27–38. https://doi.org/10.1016/j.npep.2017.01.001
Weerakoon, P., O’Sullivan, V., 1998. Inappropriate Patient Sexual Behaviour in Physiotherapy Practice. Physiotherapy 84, 491–499. https://doi.org/10.1016/S0031-9406(05)65869-5
WHO, 2002. ICF Beginner’s Guide: Towards a Common Language for Functioning, Disability and Health [WWW Document]. URL https://www.who.int/publications/m/item/icf-beginner-s-guide-towards-a-common-language-for-functioning-disability-and-health (accessed 3.29.24).
BIBLIOGRAFIA
AIFI, 2011. Codice Deontologico | A.I.FI. [WWW Document]. https://aifi.net/. URL https://aifi.net/professione/codice-deontologico/ (accessed 1.21.24).
Amanulla, S., Saju, I., Solé, S., Campoy, C., Martínez, L., Pérez-Yus, M.C., Sitjà-Rabert, M., Serrat, M., Bravo, C., Lo, K., 2021. Inappropriate Patient Sexual Behavior in Physiotherapy: A Systematic Review. Sustainability 13, 13876. https://doi.org/10.3390/su132413876
Ang, A.Y.-C., DipPhys, I.C.G., DipPhys, S.J.G., 2010. Sexual professional boundaries: physiotherapy students’ experiences and opinions 38.
APTA, 2019. Standards of Ethical Conduct for the Physical Therapist Assistant [WWW Document]. URL https://www.apta.org/apta-and-you/leadership-and-governance/policies/standards-of-ethical-conduct-for-the-physical-therapist-assistant (accessed 1.15.24).
Aravind, V.K., Krishnaram, V.D., Thasneem, Z., 2012. Boundary Crossings and Violations in Clinical Settings. Indian J Psychol Med 34, 21–24. https://doi.org/10.4103/0253-7176.96151
Boissonnault, J.S., Cambier, Z., Hetzel, S.J., 2019. Inappropriate Patient Sexual Behavior When Working in Sensitive Areas of the Body: Results From a National Physical Therapy Survey. The Journal of Women’s & Pelvic Health Physical Therapy 43, 36. https://doi.org/10.1097/JWH.0000000000000118
Boissonnault, J.S., Cambier, Z., Hetzel, S.J., Plack, M.M., 2017. Prevalence and Risk of Inappropriate Sexual Behavior of Patients Toward Physical Therapist Clinicians and Students in the United States. Physical Therapy 97, 1084–1093. https://doi.org/10.1093/ptj/pzx086
Bowen, E., Nayfe, R., Milburn, N., Mayo, H., Reid, M.C., Fraenkel, L., Weiner, D., Halm, E.A., Makris, U.E., 2020. Do Decision Aids Benefit Patients with Chronic Musculoskeletal Pain? A Systematic Review. Pain Med 21, 951–969. https://doi.org/10.1093/pm/pnz280
Cambier, Z., 2013. Preparing New Clinicians to Identify, Understand, and Address Inappropriate Patient Sexual Behavior in the Clinical Environment: Journal of Physical Therapy Education 27, 7–14. https://doi.org/10.1097/00001416-201301000-00003
Cambier, Z., Boissonnault, J.S., Hetzel, S.J., Plack, M.M., 2018. Physical Therapist, Physical Therapist Assistant, and Student Response to Inappropriate Patient Sexual Behavior: Results of a National Survey. Physical Therapy 98, 804–814. https://doi.org/10.1093/ptj/pzy067
College of Psychologist of Ontario, 2024. Professional Boundaries in Health-Care Relationships – CPO Public. URL https://cpo.on.ca/cpo_resources/professional-boundaries-in-health-care-relationships/ (accessed 1.20.24).
Cooper, I., Jenkins, S., 2008. Sexual boundaries between physiotherapists and patients are not perceived clearly: an observational study. Australian Journal of Physiotherapy 54, 275–279. https://doi.org/10.1016/S0004-9514(08)70007-2
Cooper, I., Jones, A., Jenkins, S., 2010. Professional sexual boundaries—Asian and Western perception: An observational study. Hong Kong Physiotherapy Journal 28, 2–10. https://doi.org/10.1016/j.hkpj.2010.11.003
Cullen, R.M., 1996. Sexual contact in the professional relationship : the 1996 survey of NZSP members [WWW Document]. New Zealand journal of physiotherapy,NZ journal of physiotherapy Aug 1997; v.25 n.2:p.7-9; issn: URL https://natlib.govt.nz/records/21056446 (accessed 1.15.24).
deMayo, R.A., 1997. Patient Sexual Behaviors and Sexual Harassment: A National Survey of Physical Therapists. Physical Therapy 77, 739–744. https://doi.org/10.1093/ptj/77.7.739
Geri, T., Viceconti, A., Minacci, M., Testa, M., Rossettini, G., 2019. Manual therapy: Exploiting the role of human touch. Musculoskelet Sci Pract 44, 102044. https://doi.org/10.1016/j.msksp.2019.07.008
Glass, L.L., 2003. The gray areas of boundary crossings and violations. Am J Psychother 57, 429–444. https://doi.org/10.1176/appi.psychotherapy.2003.57.4.429
Gutheil, T.G., Gabbard, G.O., 1998. Misuses and misunderstandings of boundary theory in clinical and regulatory settings. Am J Psychiatry 155, 409–414. https://doi.org/10.1176/ajp.155.3.409
Gutheil, T.G., Gabbard, G.O., 1993. The concept of boundaries in clinical practice: theoretical and risk-management dimensions. Am J Psychiatry 150, 188–196. https://doi.org/10.1176/ajp.150.2.188
Higgs, J., Refshauge, K., Ellis, E., 2001. Portrait of the physiotherapy profession. J Interprof Care 15, 79–89. https://doi.org/10.1080/13561820020022891
McComas, J., Hébert, C., Giacomin, C., Kaplan, D., Dulberg, C., 1993. Experiences of Student and Practicing Physical Therapists With Inappropriate Patient Sexual Behavior. Physical Therapy 73, 762–769. https://doi.org/10.1093/ptj/73.11.762
McComas, J., Kaplan, D., Giacomin, C., 1995. Inappropriate patient sexual behaviour in physiotherapy practice: a qualitative analysis of questionnaire comments. Physiother Can 47, 127–133.
O’Sullivan, V., Weerakoon, P., 1999. Inappropriate sexual behaviours of patients towards practising physiotherapists: a study using qualitative methods. Physiotherapy Res Intl 4, 28–42. https://doi.org/10.1002/pri.1999.4.1.28
Physiotherapy Board of New Zealand, 2023. Professional boundaries standard [WWW Document]. Mercury IT. URL https://www.physioboard.org.nz/standards/physiotherapy-standards/professional-boundaries-standard (accessed 1.20.24).
Plaut, S., 2008. Sexual and nonsexual boundaries in professional relationships: Principles and teaching guidelines. Sexual and Relationship Therapy 23, 85–94. https://doi.org/10.1080/14681990701616624
Pope, K.S., Vasquez, M.J., 2007. Ethics in Psychotherapy and Counseling: A Practical Guide. John Wiley & Sons.
Poulis, I., 2007. Bioethics and physiotherapy. J Med Ethics 33, 435–436. https://doi.org/10.1136/jme.2007.021139
Roush, S.E., Cox, K., Garlick, J., Kane, M., Marchand, L., 2015. Physical therapists’ perceptions of sexual boundaries in clinical practice in the United States. Physiotherapy Theory and Practice 31, 327–336. https://doi.org/10.3109/09593985.2014.1003420
Soundy, A., Stubbs, B., Jenkins, S., Cooper, I., 2013. Sexual professional boundaries perceived by undergraduate and graduate physiotherapists: A cross sectional survey. Physiotherapy 99, 298–304. https://doi.org/10.1016/j.physio.2012.12.005
TSRM PSTRP, 2021. Costituzione-etica-FNO-TSRM-e-PSTRP-def.pdf [WWW Document]. URL https://www.tsrm-pstrp.org/wp-content/uploads/2021/11/Costituzione-etica-FNO-TSRM-e-PSTRP-def.pdf (accessed 1.21.24).
Weerakoon, P., O’Sullivan, V., 1998. Inappropriate Patient Sexual Behaviour in Physiotherapy Practice. Physiotherapy 84, 491–499. https://doi.org/10.1016/S0031-9406(05)65869-5