Efficacy of spinal high-velocity-low-amplitude thrust manipulations in patients with radiculopathy: a systematic review with meta-analysis of randomized controlled studies
Autori
Giuseppe Giovannico [Department of Medicine and Health Science “Vincenzo Tiberio”, University of Molise, Campobasso, Italy]
Matteo Cioeta [Department of Medicine and Health Science “Vincenzo Tiberio”, University of Molise, Campobasso, Italy]
Gabriele Giannotta [Associazione “La Nostra Famiglia” – IRCCS "E. Medea" – Unit for Severe disabilities in developmental age and young adults (Developmental Neurology and Neurorehabilitation) – Brindisi, Italy]
Silvia Bargeri [IRCCS Istituto Ortopedico Galeazzi, Unit of Clinical Epidemiology, Milan, Italy]
Fabrizio Brindisino [Department of Medicine and Health Science “Vincenzo Tiberio”, University of Molise, Campobasso, Italy]
Leonardo Pellicciari [IRCCS Istituto delle Scienze Neurologiche di Bologna, Bologna, Italy]
Background and aims
A multimodal approach, including manual therapy, is the most efficient approach for cervical, thoracic, and lumbar radiculopathy. Among manual therapy techniques spinal high-velocity-low-amplitude thrust (HVLAT) manipulation is widely used. However, the efficacy of HVLAT for cervical, thoracic, and lumbar radiculopathy remains uncertain, and a comprehensive literature review is currently lacking on the HVLAT efficacy on thoracic and lumbar radiculopathy. Therefore, this study aimed to assess the HVLAT efficacy in patients with radiculopathy.
Methods
The study protocol was a-priori registered on PROSPERO (CRD42022343394). Medline, CINAHL, EMBASE, CENTRAL, PEDro were searched from their inception until May 2024. Randomized controlled studies assessing the effect of HVLATs in adult patients with cervical, thoracic, or lumbar radiculopathy on pain intensity, disability and other clinical outcomes (range of motion [ROM], quality of life, adverse events) were included. Two independent reviewers performed the study selection, data extrapolation, assessment of risk of bias (Revised Cochrane RoB Tool 2.0), certainty of evidence (CoE) (GRADE approach) and clinical relevance (defined as an additional 20% improvement between groups based on the baseline values of our dataset). If at least two studies assessed the same outcome, meta-analyses using a random-effects model were performed with appropriate effect sizes.
Results
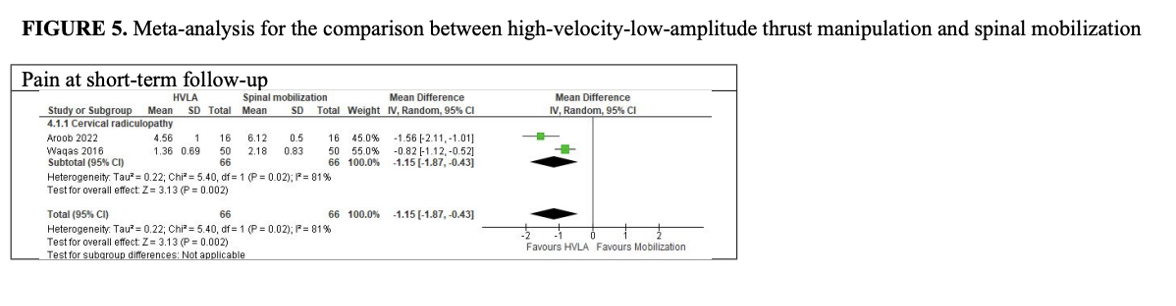
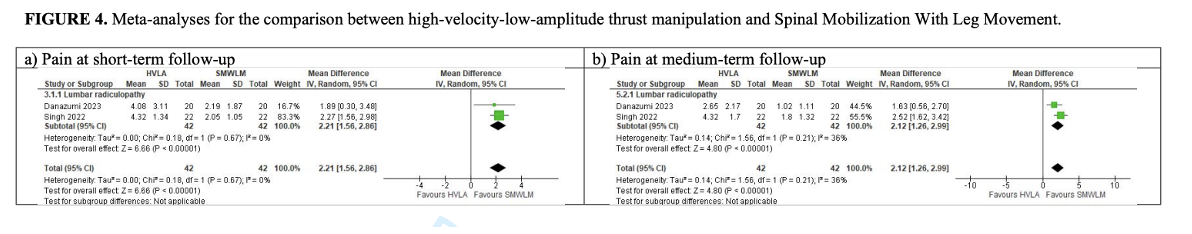
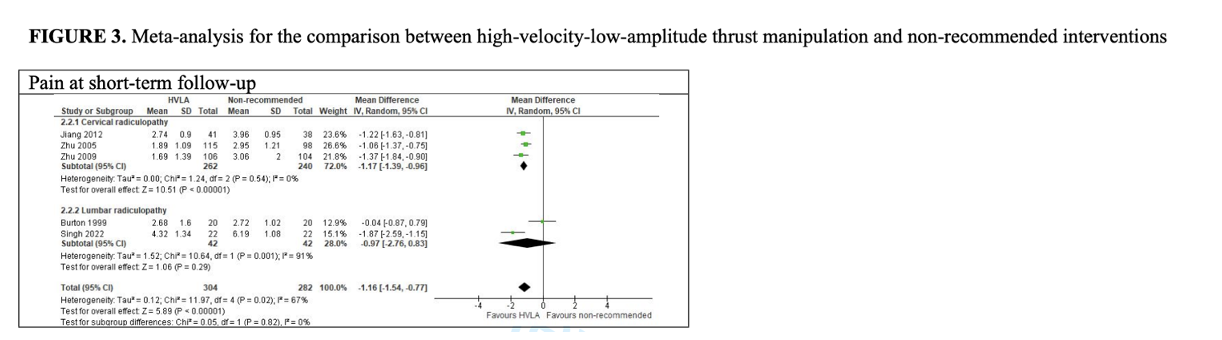
Results: Eleven RCTs (N=991), all at high RoB, were included. Compared to non-recommended interventions, there was low CoE that HVLAT may reduce pain in the short term with probable clinical relevance (MD: -1.16; 95% CI: -1.54, -0.77, five studies; 586 patients) in cervical and lumbar radiculopathy. In all other comparisons, there was low to very low CoE that HVLA may reduce pain and disability in the short and medium term, except for HVLAT vs spinal mobilization with leg movement, in which results may be in favor of the control, but the evidence is uncertain. Three studies assessed QoL with contrasting results. In two studies, control group reported greater improvements in ROM. No adverse events occurred in the three studies evaluating the outcome. No study included patients with thoracic radiculopathy.
Conclusion
HVLAT may reduce pain and disability in patients with cervical and lumbar radiculopathy in the short- and medium-terms when compared with sham HVLAT, non-recommended interventions, physiotherapy alone (when HVLAT is added to physiotherapy), and spinal mobilization, but not when compared to spinal mobilization with leg movement; however the evidence is still uncertain. Further high-quality research is needed to clarify HVLAT long-term efficacy and safety, especially for thoracic radiculopathy.
REFERENCES
1. Albrecht D, Ahmed S, Kettner N, et al. Neuroinflammation of the spinal cord and nerve 473 roots in chronic radicular pain patients. Pain. 2018;159(5):968-977. 474 doi:10.1097/j.pain.0000000000001171
2. Bialosky JE, Beneciuk JM, Bishop MD, et al. Unraveling the Mechanisms of Manual 495 Therapy: Modeling an Approach. J Orthop Sports Phys Ther. 2018;48(1):8-18. 496 doi:10.2519/jospt.2018.7476
3. Bishop MD, Mintken PE, Bialosky JE, Cleland JA. Patient expectations of benefit from 507 interventions for neck pain and resulting influence on outcomes. J Orthop Sports Phys Ther. 508 2013;43(7):457-465. doi:10.2519/jospt.2013.4492
4. Danazumi MS, Nuhu JM, Ibrahim SU, et al. Effects of spinal manipulation or 529 mobilization as an adjunct to neurodynamic mobilization for lumbar disc herniation with 530 radiculopathy: a randomized clinical trial. J Man Manip Ther. 2023;31(6):408-420. 531 doi:10.1080/10669817.2023.2192975
5. Singh V, Malik M. Effect of manual therapy on pain, disability and neural mobility in 656 patients of lumbar prolapsed intervertebral disc: a randomized controlled trial. Accessed July 25, 657 2024. https://www.advrehab.org/Effect-of-manual-therapy-on-pain-disability-and-neural658 mobility-in-patients-of-lumbar-prolapsed-intervertebral-disc-a-randomized-controlled659 trial,125,47845,0,1.html