RANGE OF MOTION AS A PROGNOSTIC FACTOR IN PATIENTS WITH SPECIFIC AND NON–SPECIFIC SPINAL PAIN: A SYSTEMATIC REVIEW
Autori
Feller Daniel (Azienda Provinciale per i Servizi Sanitari, Trento, Italia; Erasmus Medical Center, Rotterdam, The Netherlands)
Bortoli Michela (Azienda Provinciale per i Servizi Sanitari, Trento, Italia)
Rigo Adriano (Azienda Provinciale per i Servizi Sanitari, Trento, Italia)
Maini Irene (Azienda Provinciale per i Servizi Sanitari, Trento, Italia)
Hayden Jill (Dalhousie University, Halifax, Canada)
Chiarotto Alessandro (Erasmus Medical Center, Rotterdam, The Netherlands)
Background and aims
Identifying prognostic factors—variables that help predict clinical outcomes—is essential for improving patient care and guiding treatment decisions. Range of motion (ROM) is routinely assessed in clinical practice, yet its prognostic value in patients with spinal pain remains unclear. Therefore, this systematic review aimed to determine whether reduced spinal ROM predicts outcomes such as pain intensity, disability, or global recovery in individuals with specific or non-specific spinal pain.
Methods
(CRD42024583518). We included prospective and retrospective cohort studies, case-control studies, and secondary analyses of randomized controlled trials evaluating ROM as a prognostic factor in adults (≥18 years) with spinal pain. We included studies assessing active or passive ROM using any objective method. Databases searched included MEDLINE, Embase, CENTRAL, and CINAHL up to May 24, 2024. Risk of bias was assessed using the QUIPS tool, and certainty of evidence was rated using the GRADE approach. Two authors independetly performed the study selection, data extraction and risk of bias assessment phases. Due to clinical and methodological heterogeneity, results were synthesized narratively.
Results
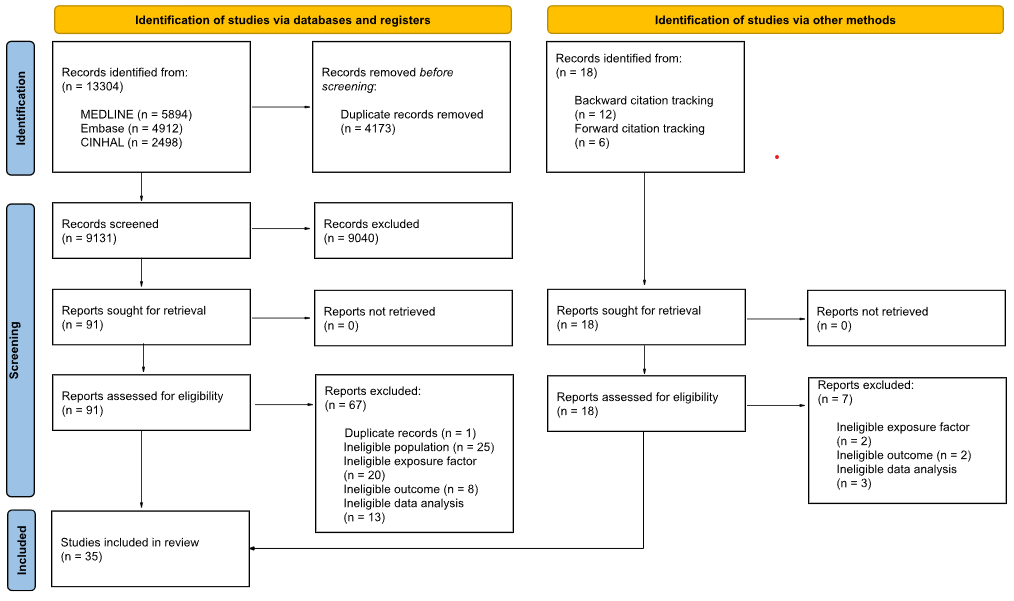
A total of 35 studies were included: 11 on acute low back pain (LBP), 10 on chronic or unspecified LBP, 4 on chronic neck pain, 2 on lumbar spinal stenosis, and 8 on whiplash-associated disorders. No studies addressed acute neck pain. ROM was most commonly measured using inclinometers and goniometers, though methods varied widely. Across all conditions, the certainty of evidence was very low due to high risk of bias (particularly inadequate adjustment for confounders), inconsistent findings, and methodological heterogeneity. While some studies reported significant associations between reduced ROM and worse outcomes (especially in whiplash and lumbar stenosis), most showed no consistent relationship. Many studies showed inadequate reporting, often presenting only statistical test results without point estimates or confidence intervals, which limits the clinical interpretability of the findings.
Conclusion
There is currently low to very low-certainty evidence that reduced spinal ROM is a prognostic factor for pain, disability, or recovery in patients with spinal pain. Therefore, routine ROM assessment may have limited value for prognosis alone. However, ROM remains clinically relevant for identifying movement-related dysfunction and informing treatment decisions. Future high-quality, prospective studies with robust adjustment for confounders are needed to clarify the independent prognostic role of spinal ROM, especially in underexplored populations such as those with acute neck pain.
REFERENCES
- Hayden JA, van der Windt DA, Cartwright JL, Côté P, Bombardier C. Assessing bias in studies of prognostic factors. Ann Intern Med. 2013 Feb 19;158(4):280-6. doi: 10.7326/0003-4819-158-4-201302190-00009. PMID: 23420236.
- Huguet A, Hayden JA, Stinson J, McGrath PJ, Chambers CT, Tougas ME, Wozney L. Judging the quality of evidence in reviews of prognostic factor research: adapting the GRADE framework. Syst Rev. 2013 Sep 5;2:71. doi: 10.1186/2046-4053-2-71. PMID: 24007720; PMCID: PMC3930077.
- Riley RD, Hayden JA, Steyerberg EW, Moons KG, Abrams K, Kyzas PA, Malats N, Briggs A, Schroter S, Altman DG, Hemingway H; PROGRESS Group. Prognosis Research Strategy (PROGRESS) 2: prognostic factor research. PLoS Med. 2013;10(2):e1001380. doi: 10.1371/journal.pmed.1001380. Epub 2013 Feb 5. PMID: 23393429; PMCID: PMC3564757.