Costochondritis syndrome and thoracic-chest related pain: a scoping review
Autori
Bolandrini Andrea [Department of Human Neuroscience, “Sapienza” University of Rome, Roma, Italy]
Barile Antonio [Department of Human Neuroscience, “Sapienza” University of Rome, Roma, Italy]
Segat Marco [Department of Human Neuroscience, “Sapienza” University of Rome, Roma, Italy; Department of Neuroscience, University of Padova, Padova, Italy]
Zaninetti Martina [Department of Human Neuroscience, “Sapienza” University of Rome, Roma, Italy]
Fascia Matteo [Department of Human Neuroscience, “Sapienza” University of Rome, Roma, Italy; Department of Information Engineering, University of Brescia, Italy]; Segat Andrea [Department of Human Neuroscience, “Sapienza” University of Rome, Roma, Italy; Department of Neuroscience, University of Padova, Padova, Italy]
Sebastiani Marta [Department of Human Neuroscience, “Sapienza” University of Rome, Roma, Italy]
Minetti Federico [Department of Human Neuroscience, “Sapienza” University of Rome, Roma, Italy]
Maselli Filippo [Department of Human Neuroscience, “Sapienza” University of Rome, Roma, Italy]
Galeoto Giovanni [Department of Human Neuroscience, “Sapienza” University of Rome, Roma, Italy]
Margelli Michele [Department of Human Neuroscience, “Sapienza” University of Rome, Roma, Italy; Department of Morphology Surgery and Experimental Medicine, Ferrara University, Ferrara, Italy]
Background and aims
Musculoskeletal chest pain is the most frequent type of chest pain encountered in primary care settings¹ and requires a comprehensive and often urgent clinical evaluation due to its heterogeneous etiology and the potential for life-threatening conditions.² Among these, costochondritis (CC) is commonly diagnosed and is also known as “costosternal syndrome”, “anterior chest wall syndrome”, and “costosternal chondrodynia”.³ This review aims to map the existing literature and provide a comprehensive overview of this condition.
Methods
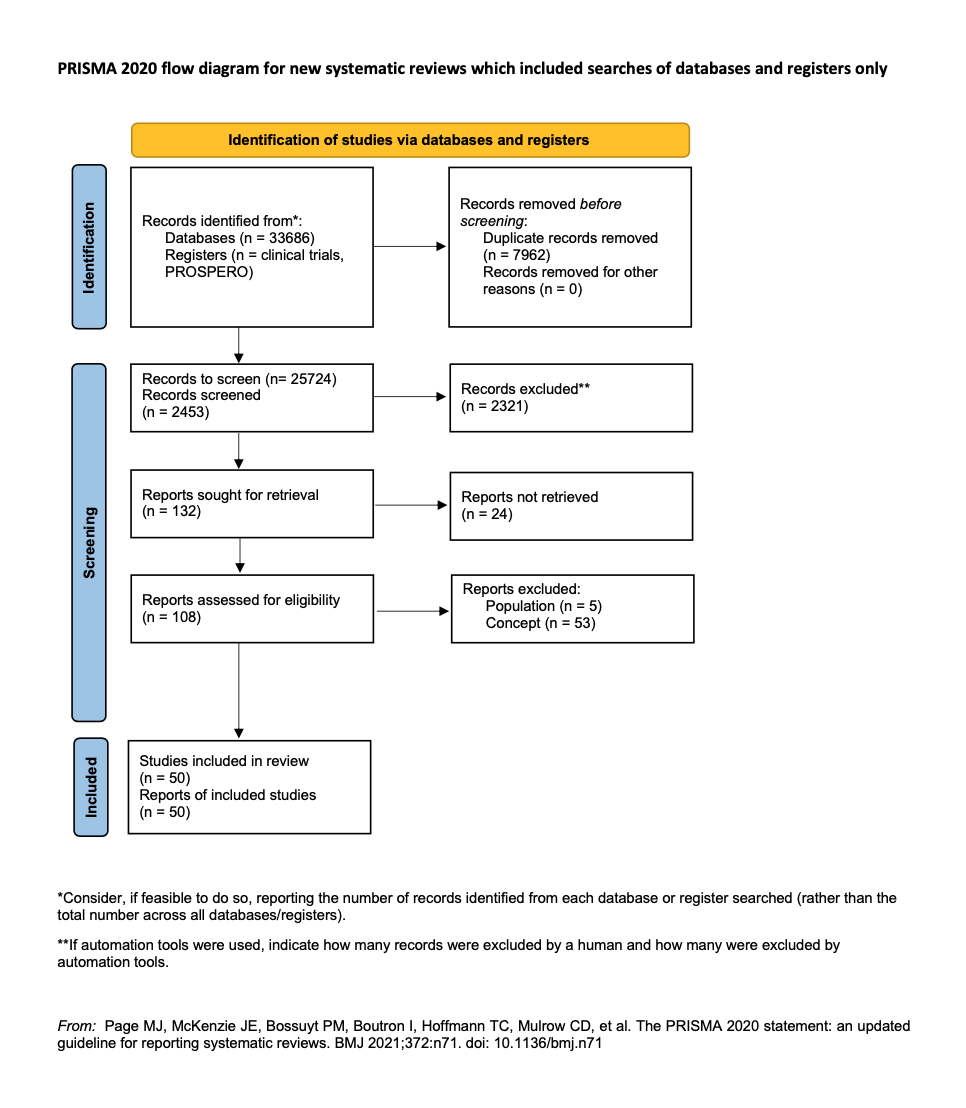
This scoping review was conducted in accordance with the PRISMA-ScR checklist 4 and the Joanna Briggs Institute methodology for scoping reviews.5 The inclusion criteria were defined using the Population, Concept, and Context (PCC) framework. Studies of any type or design, published in English or Italian, were included without restrictions on publication date or geographical location.
Results
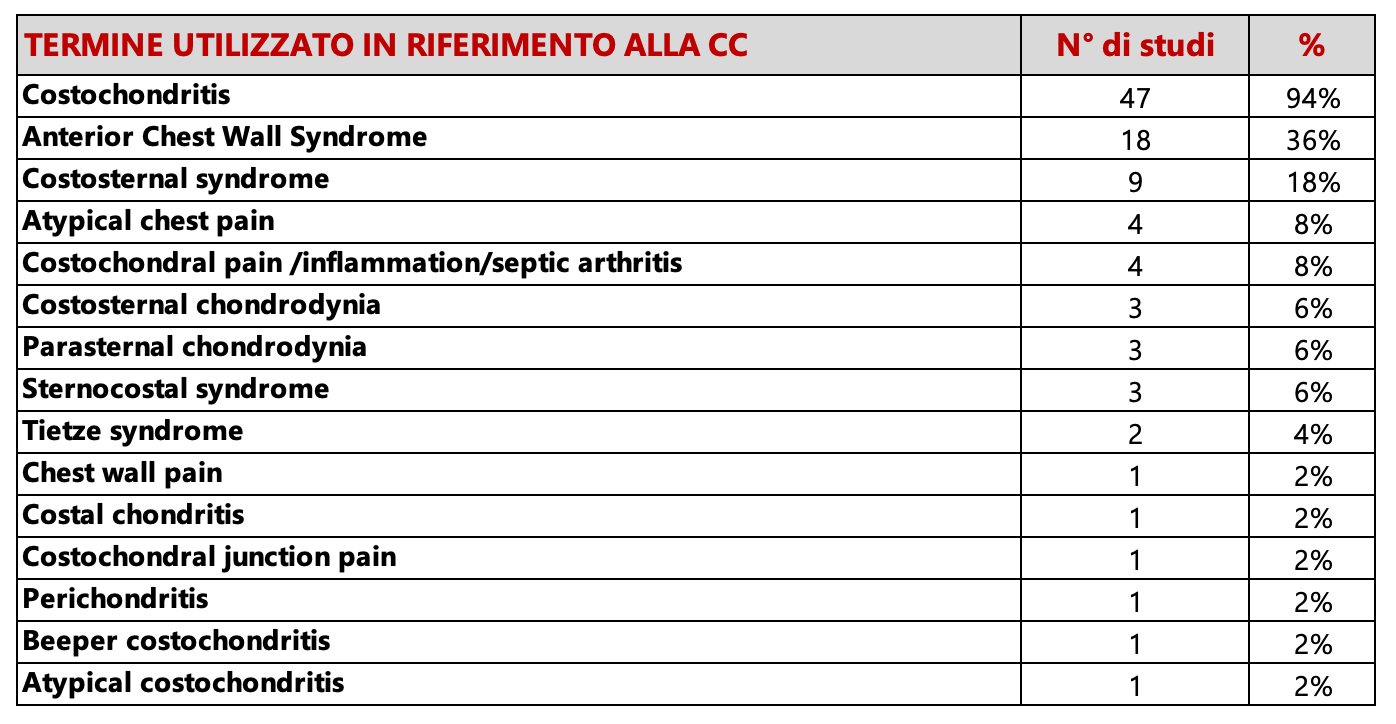
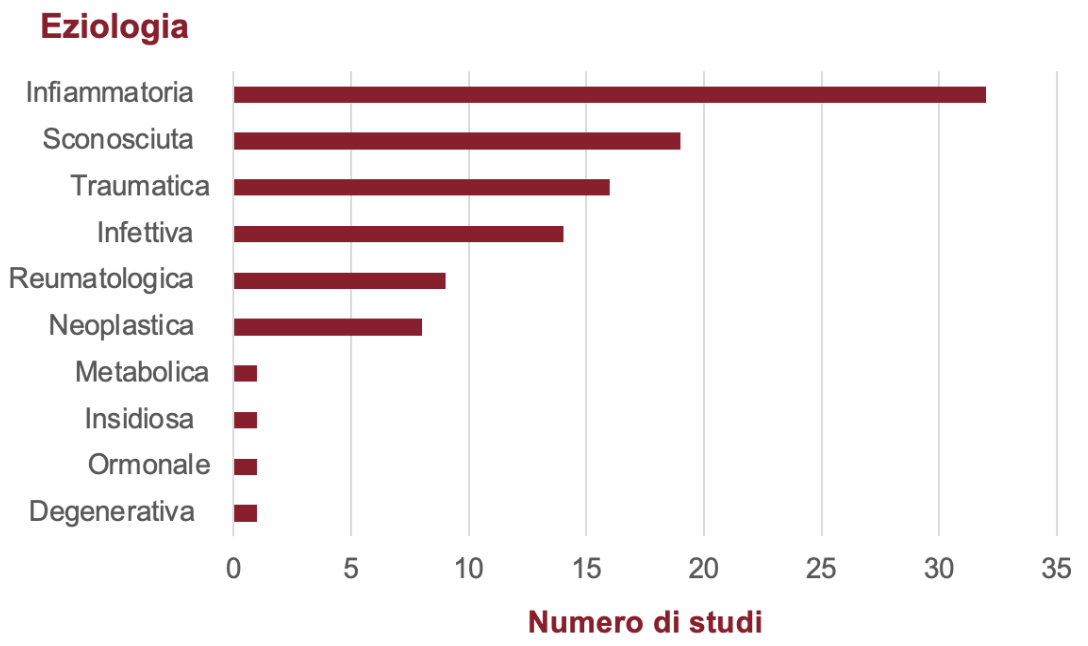
The term “costochondritis” was predominant, appearing in 94% of the studies reviewed. We identified 15 different terms used to refer to this condition, including “Tietze Syndrome”. Definitions of CC revealed discrepancies, particularly regarding the localization of pain and other features considered characteristic by some studies, such as localized tenderness and swelling. A total of 10 etiologies were identified (inflammatory, unknown, traumatic, infectious, rheumatologic, neoplastic, metabolic, insidious, hormonal, and degenerative), with multiple potential causes simultaneously reported in 56% of the studies. The most frequently reported etiology was inflammation (64%); however, this scoping review did not identify any studies demostrating the presence of an inflammatory process in individuals affected by CC.
Conclusion
This scoping review is the first to highlight the heterogeneity in terminology and the inconsistencies in the definitions of this condition. The interchangeable use of “Tietze syndrome” and “costochondritis” increases the risk of confusing the two pathological entities. The findings also underscore the lack of consistent evidence supporting the presence of a clear inflammatory process in this condition.
REFERENCES
- Stochkendahl MJ, Christensen HW. Chest pain in focal musculoskeletal disorders. Med Clin North Am. 2010 Mar;94(2):259-73. doi: 10.1016/j.mcna.2010.01.007. PMID: 20380955.
- Winzenberg T, Jones G, Callisaya M. Musculoskeletal chest wall pain. Aust Fam Physician. 2015 Aug;44(8):540-4. PMID: 26510139.
- Proulx AM, Zryd TW. Costochondritis: diagnosis and treatment. Am Fam Physician. 2009 Sep 15;80(6):617-20. PMID: 19817327.
- Tricco AC, Lillie E, Zarin W, O’Brien KK, Colquhoun H, Levac D, Moher D, Peters MDJ, Horsley T, Weeks L, Hempel S, Akl EA, Chang C, McGowan J, Stewart L, Hartling L, Aldcroft A, Wilson MG, Garritty C, Lewin S, Godfrey CM, Macdonald MT, Langlois EV, Soares-Weiser K, Moriarty J, Clifford T, Tunçalp Ö, Straus SE. PRISMA Extension for Scoping Reviews (PRISMA-ScR): Checklist and Explanation. Ann Intern Med. 2018 Oct 2;169(7):467-473. doi: 10.7326/M18-0850. Epub 2018 Sep 4. PMID: 30178033.
- Aromataris, E., Lockwood, C., Porritt, K., Pilla, B., & Jordan, Z. (Eds.).(2024). JBI Manual for Evidence Synthesis. JBI. https://doi.org/10.46658/JBIMES-24-01