Psychometric properties of the Mini-Balance Evaluation Systems Test (Mini-BESTest) in stroke patients: a systematic review
Autori
Lazzaro Alberto [Aulss 6 Euganea, Padova, IT]
Feller Daniel [Azienda Provinciale Servizi Sanitari di Trento, Trento, IT; Erasmus University Medical Center, Rotterdam, NL]
Maffei Andrea [Azienda ospedaliera dell’Alto Adige Sabes, Bolzano, IT]
Background and aims
Stroke is one of the main neurological conditions that results in impaired postural and balance control, adversely affecting multiple physiological and body systems. Over 80% of individuals who experienced a first-time stroke exhibits balance impairments, leading to a reduced ability to maintain sitting, standing, or stepping balance. Lack of postural control in people with stroke is largely recognized as negatively impacting ambulatory stability, activity of daily living, social participation, quality of life, and risk of falling.
A consensus-based paper suggests that the Mini-BESTest should be included in the minimum data set for measuring balance in adults with, and without, neurological conditions.
No systematic review analyzing the properties Mini-BESTest in the specific stroke population have been found. It is important to evaluate the psychometric properties of an assessment tool before its administration in clinical practice. Thus, the aim of this systematic review is to synthesize the psychometric properties of the Mini-BESTest in stroke subjects.
Methods
The literature search was performed in six databases in September 2024. This review included all studies reporting at least one psychometric property of the Mini-BESTest as defined by COSMIN. The PRISMA-COSMIN for outcome measurement instruments were used for the reporting of the studies. COSMIN Risk of Bias checklist version 3.0 was used to assess the methodological quality of the studies.
The protocol of the review has been registered in PROSPERO (ID: CRD42025637127).
Results
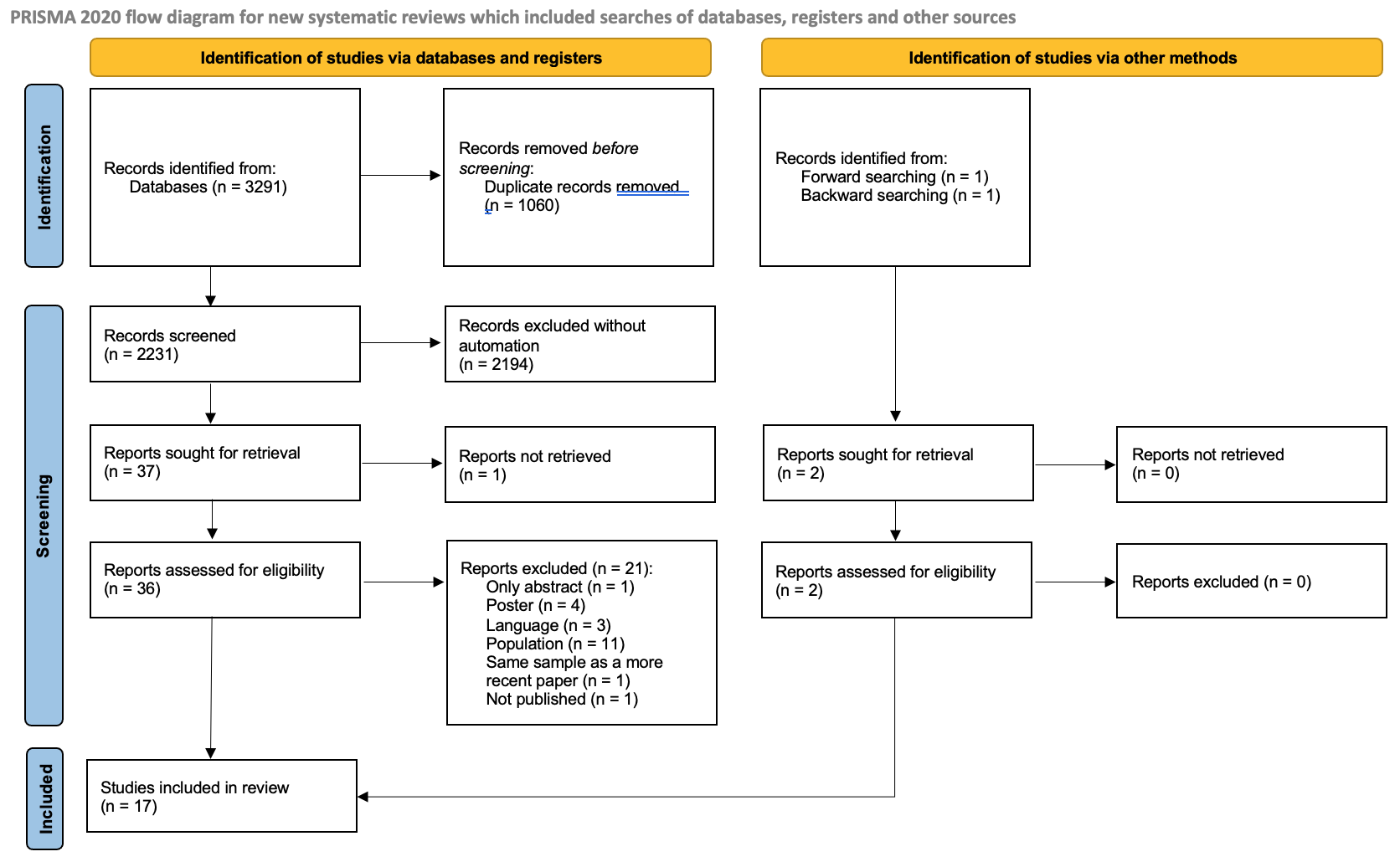
17 articles were included after the screening procedure, through a double-blind selection. Inter-rater, intra-rater and test-retest reliability were excellent. The Mini-BESTest showed good to very good internal consistency. MDC across the studies ranged from 2,01 to 4,25 and the SEM from 0,46 to 1,53. The Mini-BESTest showed an acceptable predictive validity for gait independence and risk of fall. The Mini-BESTest showed also good structural and convergent validity. Statistically significant differences in scores were found between healthy and stroke subjects and between fallers-and non-fallers, indicating a good discriminative validity. Mini-BESTest showed good to moderate responsiveness. Significant floor effect was reported in 2 studies at the baseline.
Conclusion
The Mini-BESTest represents an appropriate measurement instrument for assessing balance function in stroke patients. It has an excellent internal consistency, very good reliability, good convergent/divergent validity, high sensitivity in detecting change, no significant ceiling effect and a low to moderate floor effect.
REFERENCES
Elsman EBM, Mokkink LB, Terwee CB, Beaton D, Gagnier JJ, Tricco AC, Baba A, Butcher NJ, Smith M, Hofstetter C, Lee Aiyegbusi O, Berardi A, Farmer J, Haywood KL, Krause KR, Markham S, Mayo-Wilson E, Mehdipour A, Ricketts J, Szatmari P, Touma Z, Moher D, Offringa M. Guideline for reporting systematic reviews of outcome measurement instruments (OMIs): PRISMA-COSMIN for OMIs 2024. J Clin Epidemiol. 2024 Sep;173:111422. doi: 10.1016/j.jclinepi.2024.111422. Epub 2024 Jul 9. PMID: 38849061.
Franchignoni F, Horak F, Godi M, Nardone A, Giordano A. Using psychometric techniques to improve the Balance Evaluation Systems Test: the mini-BESTest. J Rehabil Med. 2010 Apr;42(4):323-31. doi: 10.2340/16501977-0537. PMID: 20461334; PMCID: PMC3228839.
King L, Horak F. On the mini-BESTest: scoring and the reporting of total scores. Phys Ther. 2013 Apr;93(4):571-5. doi: 10.2522/ptj.2013.93.4.571. PMID: 23547173.
Mokkink LB, Elsman EBM, Terwee CB. COSMIN guideline for systematic reviews of patient-reported outcome measures version 2.0. Qual Life Res. 2024 Nov;33(11):2929-2939. doi: 10.1007/s11136-024-03761-6. Epub 2024 Aug 28. PMID: 39198348; PMCID: PMC11541334.
Sibley KM, Howe T, Lamb SE, Lord SR, Maki BE, Rose DJ, Scott V, Stathokostas L, Straus SE, Jaglal SB. Recommendations for a core outcome set for measuring standing balance in adult populations: a consensus-based approach. PLoS One. 2015 Mar 13;10(3):e0120568. doi: 10.1371/journal.pone.0120568. PMID: 25768435; PMCID: PMC4358983.