Fatigue can influence the development of late-onset pain in post COVID-19 syndrome. An observational study.
Introduction
Coronavirus disease (COVID-19) is an infection caused by the SARS-CoV-2 virus resulting in various pathology phenotypes characterized by different symptom severities. Pain is one of the most described persistent symptoms following SARS-CoV-2 infection (Bakılan et al., 2021; Fernandez-de-Las-Penas et al., 2022; Soares et al., 2021). Causes of pain persistence after COVID-19 infection are poorly established, and different pathogenetic mechanisms have been proposed. Identifying the main features of post-COVID-19 pain is necessary to provide tailored rehabilitative interventions (Fernández-de-las-Peñas et al., 2022). For these reasons, the primary aim of this paper is to identify possible demographic-pathological features and/or clinical signs related to late-onset pain in people one year after COVID-19 infection.
Methods
This observational study was approved by the local Ethical Committee and registered on Clinicaltrials.gov. We enrolled patients with a diagnosis of COVID-19 with rehabilitation needs during the acute phase, and with an increase in pain intensity at 52 weeks from the infection’s onset compared to the pre-COVID-19 condition. All the subjects were monitored through periodic screening of post-COVID syndrome using C19-YRS at 12, 26, and 52 weeks. The subjects were evaluated with the Numeric Pain Rating Scale (NPRS), the Leeds Assessment of Neuropathic Symptoms and Signs (LANSS), the Central Sensitization Inventory (CSI), the Pain Catastrophizing Scale (PCS), the Tampa Scale of Kinesiophobia (TSK). The evaluation of the pressure pain threshold (PPT) and temporal summation (TS) was performed in COVID-19 patients and age- and sex-matched controls.
Results
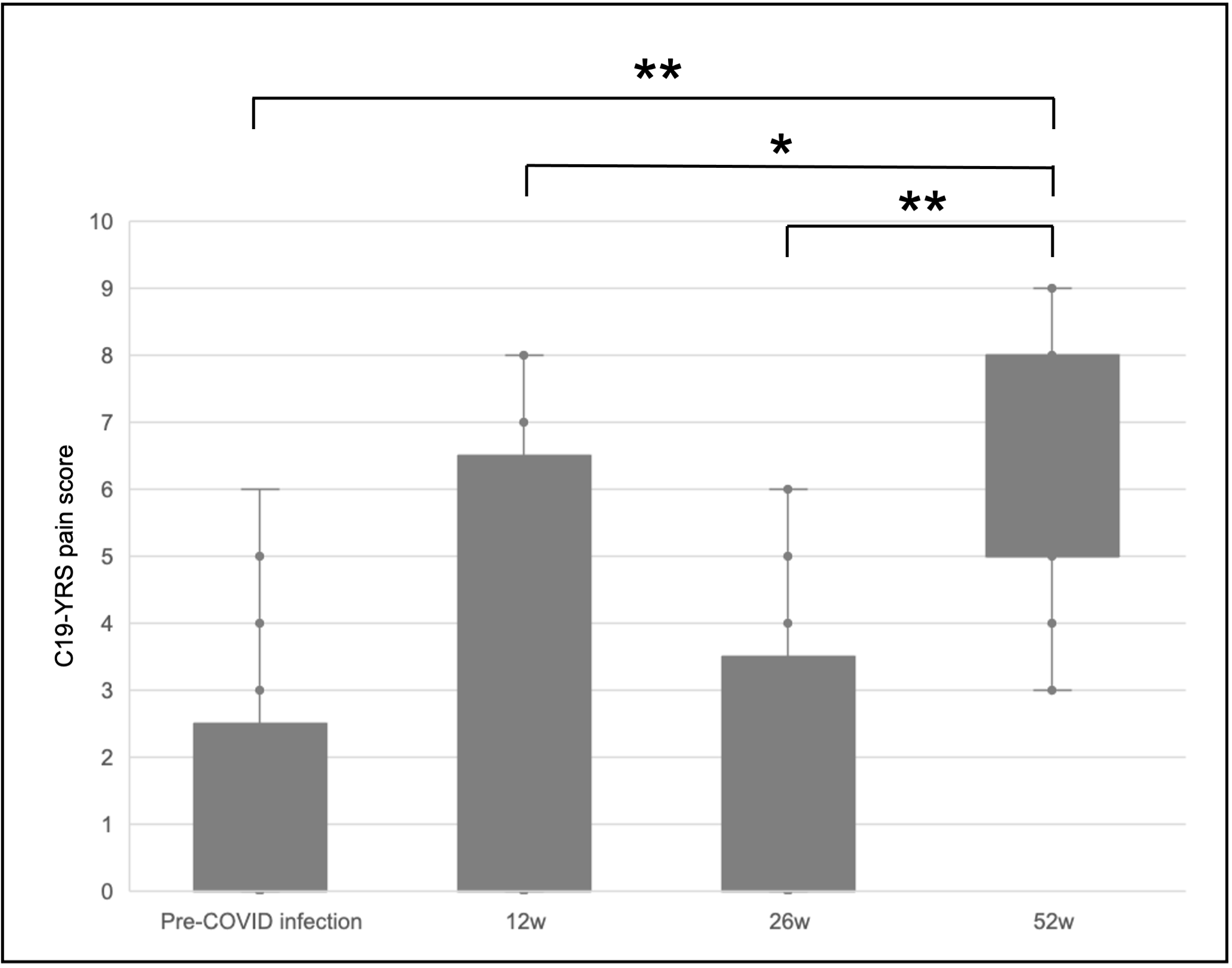
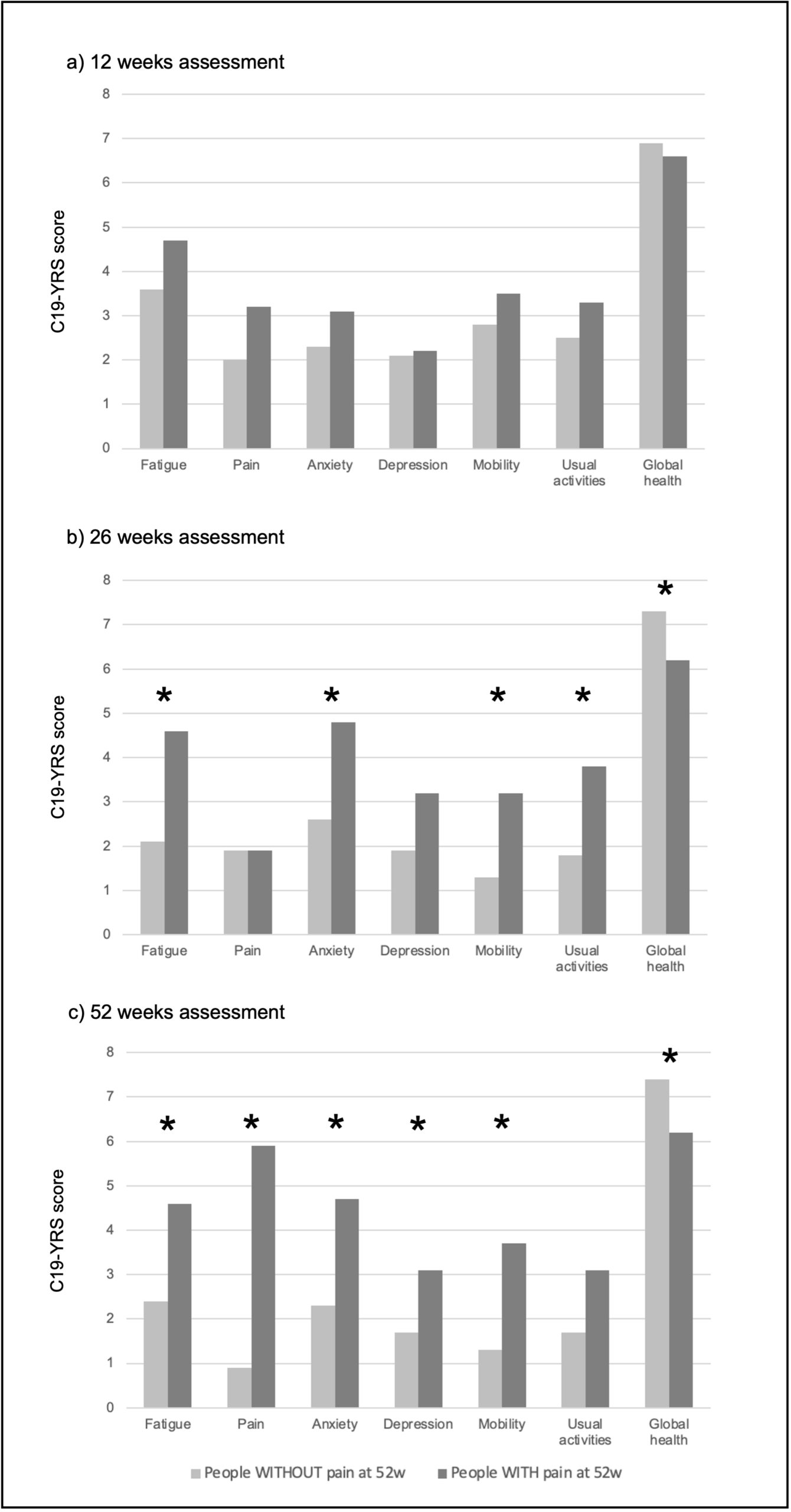
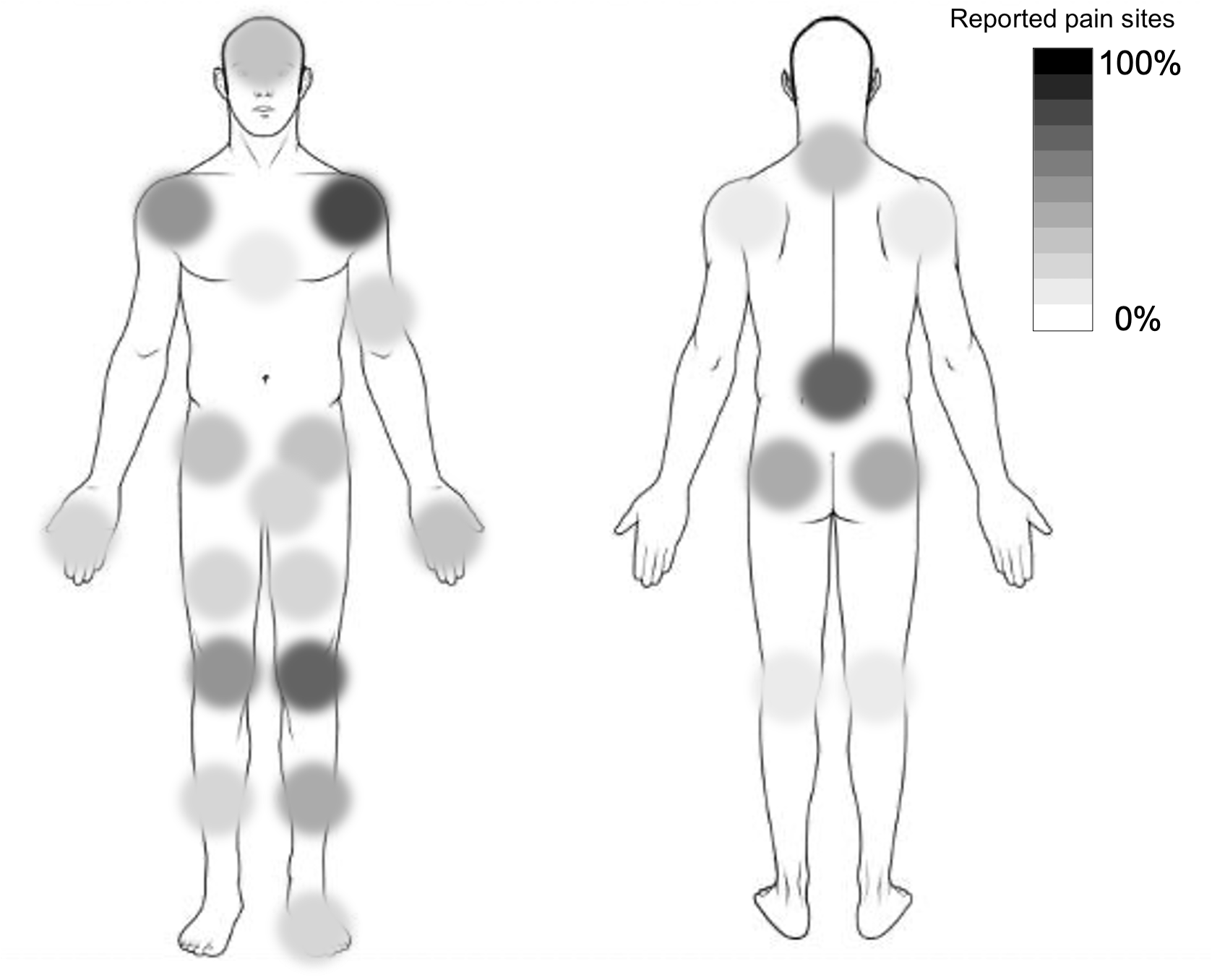
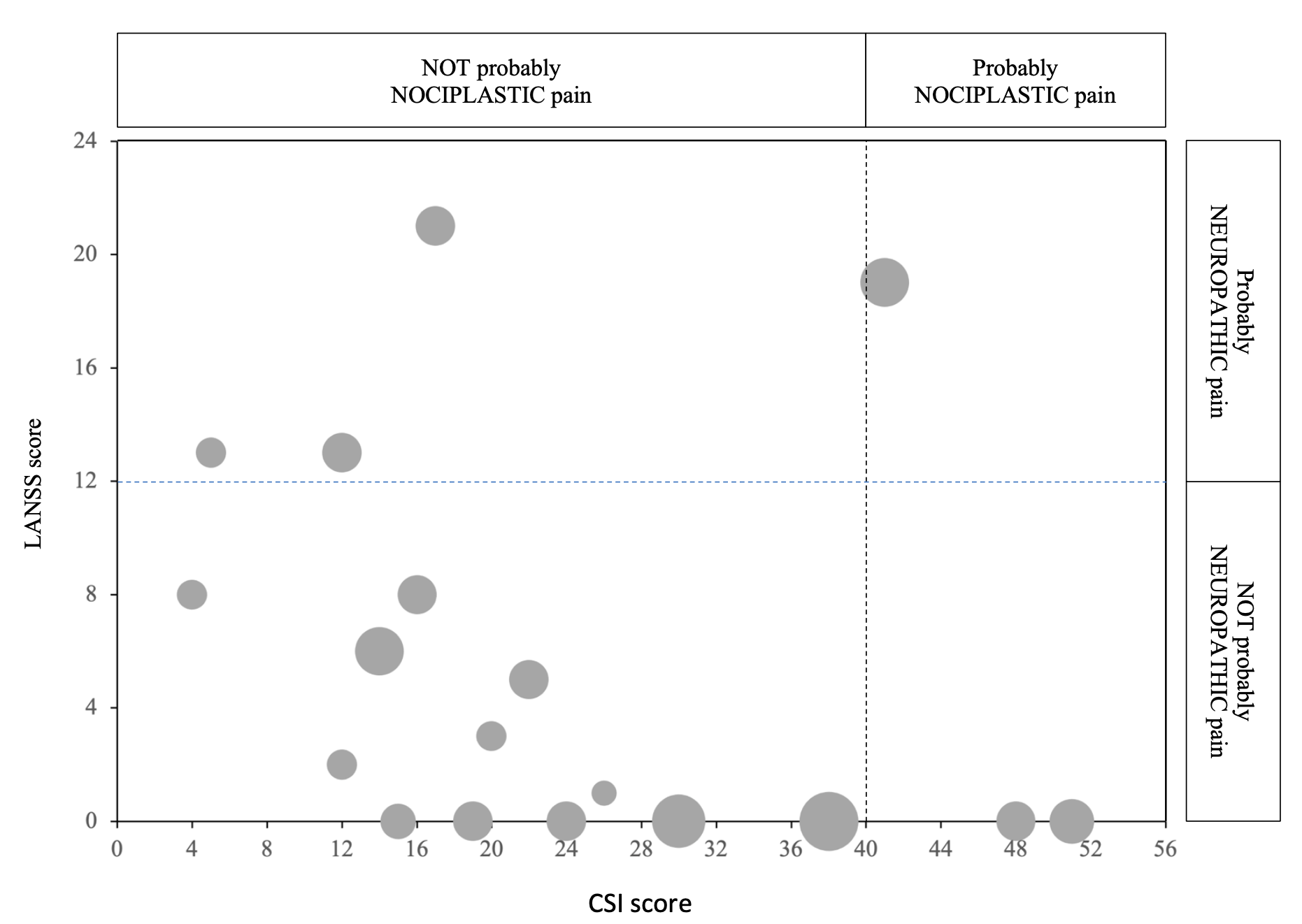
Sixty-seven patients completed the evaluation for post-COVID-19 symptoms at 52 weeks. Twenty subjects presented increased in pain intensity >= 2 points at the 52-week C19-YRS pain assessment (Fig. 1). Subjects with and without pain were similar in demographic and clinical characteristics. Comparison of C19-YRS domains at the threetime points (12, 26, 52 weeks) revealed significantly worse outcomes in fatigue, anxiety, mobility, ability to perform usual daily activities and generally health perception. Reduction in all these domains was retained at the 52-week evaluation (Fig. 2). Multiple linear regression revealed that fatigue at 26 weeks significantly predicted pain onset (b = 0.51, p = 0.006). A mean intensity of pain of 6.0 ± 1.9 was recorded; most of the sample did not show possible neuropathic or nociplastic mechanisms (Fig. 4). No differences were found in PPT and TS between subjects with pain and healthy subjects.
Discussion and Conclusion
Our study found that almost one out of three patients hospitalized for COVID-19 developed pain 52 weeks after symptom resolution. Pain intensity seems to fluctuate during the first year following COVID-19 infection. Probably the development of pain long after COVID-19 resolution may be due to new mechanisms developed months after infection, not imputable to nociceptive pathway stimulation or central sensitization (Fernandez-de-Las-Penas et al., 2022). Pain perception seems to be influenced by fatigue. This causal relationship may open the doors to new treatment approaches in pain management, targeting fatigue for late-onset pain treatment. Distinguishing between mechanisms of pain is challenging, and an overlapping is frequent. A comprehensive approach following a biopsychosocial model must consider all possible factors related to pain development, acting on the components of a vicious circle where fatigue and mood disorders play a crucial role in pain development and maintenance.
REFERENCES
– Bakılan F, Gökmen İG, Ortanca B, et al. Musculoskeletal symptoms and related factors in postacute COVID-19 patients. Int J Clin Pract. 2021;75(11):e14734. doi:10.1111/ijcp.14734
– Fernández-de-Las-Peñas C, Cancela-Cilleruelo I, Moro-López-Menchero P, et al. Exploring the trajectory curve of long-term musculoskeletal post-COVID pain symptoms in hospitalized COVID-19 survivors: a multicenter study. Pain. 2023;164(2):413-420. doi:10.1097/j.pain.0000000000002718
– Fernández-de-Las-Peñas C, Nijs J, Neblett R, et al. Phenotyping Post-COVID Pain as a Nociceptive, Neuropathic, or Nociplastic Pain Condition. Biomedicines. 2022;10(10):2562. Published 2022 Oct 13. doi:10.3390/biomedicines10102562
– Soares FHC, Kubota GT, Fernandes AM, et al. Prevalence and characteristics of new-onset pain in COVID-19 survivours, a controlled study. Eur J Pain. 2021;25(6):1342-1354. doi:10.1002/ejp.1755